  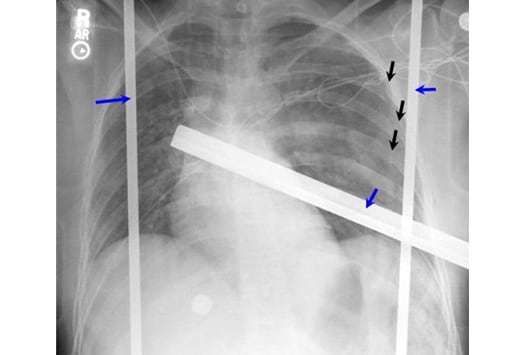 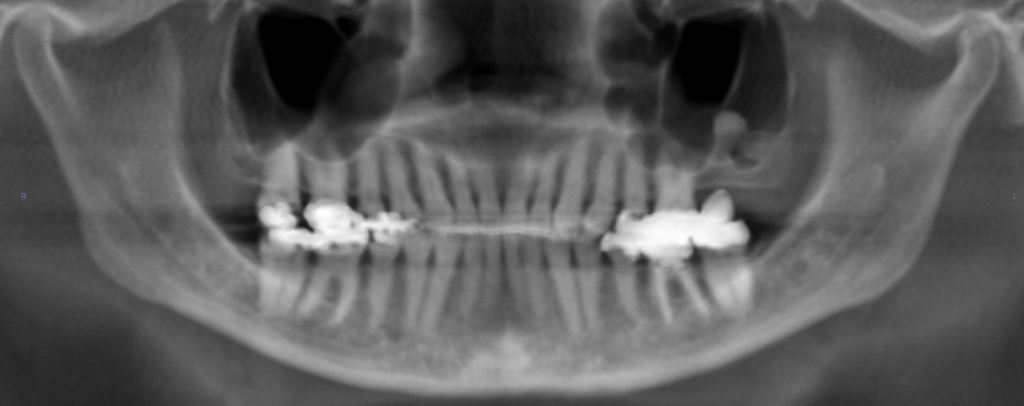
When the individual images were stitched together, the different projections of the screw were both visible. A pedicle screw was positioned in the overlapping region of the two projections. In the scoliosis examination shown in Figure 2, two radiographs were acquired with synchronous step movement of the x-ray tube and detector as previously described. When the adjacent exposures are combined, the resultant image will overlay and blend the two projections of the same anatomy, potentially resulting in image artifacts. Anatomy in the overlap region of the x-ray beam will be projected downward in the upper x-ray tube position and projected upward in the lower x-ray tube position. Individual projection images acquired at each tube-detector position are then automatically assembled into a single composite image at the modality workstation on the basis of anatomy or marking from a lead ruler imaged with the patient.Īs shown in Figure 1, to include all patient anatomy, regions near the top and bottom edge of the detector are included in two adjacent image acquisitions. In DR, one of the available methods creates a single image of long anatomy using a synchronous step movement of the x-ray tube and detector. After the imaging plates are read out, the images are combined on the basis of fiducial markings that appear in the images and indicate the location of the overlap. The plates are stationary and a single x-ray exposure is used to expose either two or three plates. The plates are overlapped to provide information across plate boundaries. To create a long image using CR, multiple cassettes are arranged into a single holder. 1 ?Schematic shows movement of x-ray beam and flat-panel detectors in digital radiography system that is set up for image compositing. Other work has also discussed DR-specific artifacts. Many different types of artifacts common to both CR and DR, including under- and overexposure (dose creep), collimation issues, and Moir? artifacts related to grid use have been covered elsewhere and will not be readdressed here. Our hope is to help expedite the discovery and resolution of DR problems and to provide guidance into what can be controlled or resolved, what is clinically significant, and what might have to be expected and accepted from different DR systems. In this article, we present our experiences with different artifacts that have arisen in our work with different DR systems over the course of several years. Establishing standard tests and control limits to identify or prevent clinically relevant artifacts can be challenging. Even if vendors use the same physical detector hardware, differences in calibration or image processing may yield different results or risk for artifacts. The recommended techniques for minimizing these artifacts can sometimes negate potential efficiency gains of DR compared with CR.Įach different DR system model and usage has the prospect for a different manifestation or degree of artifact. In using the term ?artifact,? we also include issues, such as image lag, that are related to inherent physical limitations of the detectors. Along with potential differences in efficiency, there are differences in acquisition and processing between DR and CR that can create image artifacts that are unique to DR. With the potential for patient dose reduction, increased workflow, and improved image quality, many radiology practices are purchasing flat-panel digital radiography (DR) systems instead of the more ubiquitous computed radiography (CR) systems. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
